Our daughter came unexpectedly at 35 weeks. My pregnancy wasn’t the easiest of the 4 as my blood pressure was an issue after 25 weeks causing me to have to do antenatal appointments once a week after 30 weeks with week 35 being the most eventful after being told my blood pressure was dangerously high and they needed to risk a premature baby to ensure I was safe but our little Brooklynn was born perfectly healthy, happy and strong – a strength we didn’t know she would need more than anything else.
We began noticing something was a little off after Brooklynn transitioned 100% to bottle feeds after she continued to latch poorly into her 4th week. When she would eat from a bottle, she would make what we could only describe as a “gasping” or “clearing your throat noise”. When we brought it up to the pediatrician, we were told it wasn’t an issue and she was gaining weight and thriving well. The only issue we needed to address was she unfortunately was following in her older sister’s footsteps and was showing signs of reflux.
We were prescribed Zantac and told she would likely grow out of it after a few months. After her two-month appointment, I brought Brooklynn home, fed her and had her sit up for the 20 or so minutes we had grown accustom to which helped with the reflux and spit up. Afterwards, I put her in her swing and began doing dishes. A few minutes in, I noticed Brooklynn had started her gasping noise but this time it kept going. As I looked over at her I noticed her color was changing and rushed over to see what was wrong. Was she choking? Did she pull something over her face that caused her to gasp for air? I was horrified to see her completely purple, eyes bulging and gasping for air.
I grabbed her to sit her up more only to have her go limp in my arms. Internal panic set in – I have been a CPR/First Aid/AED/Lifeguard trainer for almost 10 years and dealt with countless first aid incidents with both adult and children but NOTHING prepares you for when it is your own child.
I frantically began giving Brooklynn rescue breaths and looked for my phone which was nowhere in sight. Of all the times to not have my phone with me, this was the worst possible scenario. After what seemed like an eternity of breathing for Brooklynn and couch pillows thrown all over the floor, I heard a big gasp come out of Brooklynn and some coughs. She looked at me coughing/gasping and began to get fussy as I surveyed every part of her body to see her color returning from bluish/purple to red to normal. I found my phone buried deep in the couch as I grabbed all our things, put Brooklynn in the car and rushed to the hospital. I still remember trying to call my husband and how when he answered I barely could get words out of my mouth.
Once at the hospital, they took Brooklynn back immediately and we were told she would stay the night for observation. They called the event a BRUE (brief – resolved – unexplained – event) and said it sometimes happens but she looked good. The next day in the hospital we were blessed to have an occupational therapist who has become Brooklynn’s biggest champion through her journey notice the weird sounds she made while eating.
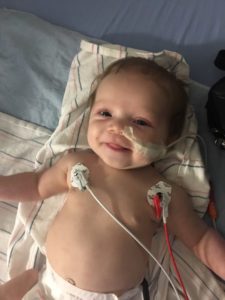
The occupational therapist pushed for further testing including a swallow study where she would be looked at under an x-ray while eating to see what was happening with her food. During this test, we were shocked to see that she was aspirating almost every time she swallowed and most were “silent aspirations” meaning she made no sound or indication that her formula was going into her airway. They immediately decided she needed a “NG – Tube” and it was not safe for her to eat by mouth. My husband and I were shaken and had no idea the turbulent path we were about to tumble down. After they placed her NG-Tube, she was still having episodes with making gasping noises so they moved to a test called a FEES study where they used a camera scope down her nose and colored formula to see exactly what was happening.
During this test it was evident, she had no control over her airway being flooded with formula – additionally, they went back to the swallow study and noticed she was even aspirating on her reflux. They then made the decision to replace her NG – Tube with a NJ – Tube, she couldn’t have anything by mouth and nothing in her stomach. After 11 days, we were sent home to begin our lives with a NJ-Tube, no answer as to why she was aspirating and the thought of many that because she was a preemie, she was probably immature in her motor skills and would grow out of it.
Fast forward to two months later after some occupational therapy visits, GI visits, and another failed swallow study. We had growing frustration with her NJ-Tube having come out 3 times and needing to be replaced at the hospital each time. I was home alone with Brooklynn and her older sister while my husband was out of town with most of our family at a wedding in Mississippi. I woke up at 2:30am to refill her bag with formula, get some water and move our daughter from the middle of our bed (only a 3-year-old finds a way to touch every inch of a king sized bed while sleeping).
As a went to move my older daughter, the all too familiar gasping nose began to come from Brooklynn who was laying in her crib next to our bed. I looked over and saw her big eyes and immediately grabbed by cell phone. As I rushed over to the other side of the bed I looked in horror to see Brooklynn turning purple again and struggling to get her breath.
I immediately called 911 as I picked her up and sat her upright, rubbed her back and tried my best to stay calm while explaining to the dispatcher what was happening. While on the phone with 911, she stopped breathing and I again found myself down on the ground breathing for her and telling her today wasn’t her day – she wasn’t going to die today.
As I continued to give her breaths and hear the dispatcher tell me the paramedics were going to be there soon (it seemed like hours were going by), I noticed a weird taste on my lips and slimy stuff on Brooklynn’s face. It hit me that something was coming from her mouth so I rolled her on her side and began scooping out of her mouth a slimy substance as she began gagging and choking – still gasping for air, I picked her up as the dispatcher told me I needed to unlock my front door. The paramedics came in and immediately grabbed my daughter and rushed her outside to the ambulance while telling me to get all my things. Our 3-year-old daughter who was awake and had watched the whole thing was crying and asking me if Brooklynn was going to be okay – I got down on my knees and told her how strong Brooklynn was and that everything was going to be okay.
They got Brooklynn stable in the ambulance and asked me to follow in our car because our other daughter couldn’t ride in the ambulance. As I followed behind the ambulance, I again called my husband and tried to get the words out to explain to him what happened. My husband began his journey home from Mississippi so he could get to the hospital as quickly as possible.
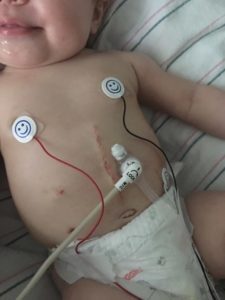
This 14 day stay in the hospital included many more tests all with no answers to her aspiration, a botched surgery where they were able to place the G-Tube but the procedure went horribly wrong during the fundoplication and they had to abort the rest of the surgery and give her blood transfusions to keep her alive. She was in the ICU for 2 days and has a large scar down her chest/belly to remind her and us how precious life can be.
What is aspiration?
Aspiration occurs whenever secretions, solid food or liquids “go down the wrong pipe” and enter the airway and lungs. Aspirating material into the lungs can lead to respiratory problems, such as pneumonia or even death. While there may be observable signs that accompany aspiration events, such as coughing, choking, eye reddening during eating, or a gurgly vocal quality after swallowing, infants and children can also aspirate “silently,” or with no observable symptoms.
Signs and risks for aspiration
- Any child with a history of recurrent pneumonia or chronic respiratory illness.
- Any child with neuromuscular disorders, both structural and functional (i.e., cerebral palsy, etc.).
- Children with excessive drooling, especially if seen to cough or gag on their own secretions.
- Infants/children with history of gastroesophageal reflux disease.
- Children who have acquired brain damage secondary to open or closed head injuries, with particular importance on those with brainstem/cranial nerve involvement.
- Infants who are born prematurely.
- Infants/children with chronic heart disease.
- Infants/children with craniofacial anomalies (i.e., cleft palate, etc.).
- Infants/children with congenital syndromes.
- Children with upper airway anomalies (i.e., congenital defects of the larynx, trachea, and esophagus; tracheoesophageal fistulas).
- Children who exhibit failure to gain weight or poor weight gain; diagnosis of failure to thrive.
- Sucking and swallowing incoordination or weak suck.
- Breathing disruption or apnea during feeding.
- Children with behavioral feeding problems (i.e., refusal to eat new foods or unexplained food refusal; rigid feeding behaviors; irritability during or after feeding).
- Children with feeding periods longer than 30 to 40 minutes.
- Children receiving enteral/tube feedings, especially under the age of 2.
- Children who exhibit aversive responses to oral stimulation
Brooklynn’s G-Tube has definitely helped as she no longer has a tube going through her nose and down her throat. We don’t have to spend our nights re-taping her or worried about it coming out. I get to see my baby’s beautiful face without a bunch of tape and she gets to be more “normal” in the sense that she can go swimming, learn to crawl, etc. without something stuck to her face. We have a long road ahead of us with genetic testing, occupational therapy, GI, ENT, and just about every other specialty appointment out there. She hasn’t been given an explanation for her diagnosis nor a timeline for how long they think this will go on for.
My advice to parents is to remember that only YOU can advocate for your child. Speak up and be persistent when you suspect something is off or isn’t right. My husband and I look back and wish we had pushed more when we began noticing something was different with Brooklynn. If you find yourself at the hospital or dealing with an unfortunate medical condition, NEVER STOP ASKING QUESTIONS and listen to your GUT – if something doesn’t feel right, it probably isn’t.
I am often told that I am so strong and I saved my daughter’s life, but the truth is that Brooklynn has more strength and fight in her than I will ever have. She has cheated death 3 times and still lights up the room with her beautiful smile and calm personality. I could only hope to have half the strength and fight for life that she possesses but I can honestly say that she has taught me a valuable lesson in the importance of unconditional and unwavering love for both my kids and my husband.
This situation, which would usually put great strain on a relationship, has only proven to both my husband and I that we wouldn’t want to be walking this journey without the other by our side. I have never felt such a strong and unbreakable fight in me than when it comes to my kids – they say you feel something unexplainable when your kids are born and I can assure you, there are no words to explain it other than a love like you will never feel anywhere else.
 Falon Leszczynski is a Manager for EXOS in San Diego. She received her degree in Human Services with an emphasis in Community Youth and Development. She has a sincere passion for building community programs that serve youth and families.
Falon Leszczynski is a Manager for EXOS in San Diego. She received her degree in Human Services with an emphasis in Community Youth and Development. She has a sincere passion for building community programs that serve youth and families.
She and her husband, Lenny, have four daughters – Addison (8), Paytyn (6), Morgan (3) and Brooklynn (4 months). They spend most of their weekends at the softball fields watching their daughters games. Falon is an avid football fan, enjoys anything in the water- unless there are sharks involved and really enjoys time with family and friends.